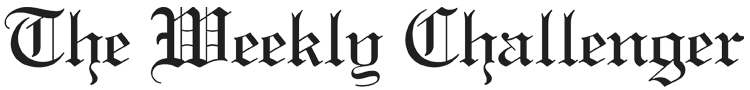Lupus disproportionately affects Black people due to a lack of information within the community and a lack of knowledge of the disease by medical professionals.
BY YOLANDA GOODLOE COWART, Contributor
Regarding our health, knowledge is the number one weapon we have to combat the vast array of diseases and illnesses plaguing the human race. Knowledge helps us know what to look out for, and it helps us understand how to advocate for proper healthcare.
With proper and adequate knowledge, we can even educate our medical practitioners and point them in the right direction in terms of prompt diagnosis and treatment. Ultimately, knowledge helps to improve our life expectancy and comfort. Without it, we end up suffering for months and sometimes years, going from one test to another.
Lupus is one such disease that disproportionately affects the Black people due to a lack of information within the community and a lack of knowledge of the disease by medical professionals. If both sides knew more about the disease and the different ways it presents itself, symptoms would likely be recognized earlier.
Without accurate information, Black men and women end up underdiagnosed and spend years bouncing from one misdiagnosis to another before landing on the correct diagnosis and receiving proper treatment.
What the Black community needs to know about lupus
Lupus is a chronic, autoimmune disease that currently has no cure. It causes a person’s immune system to attack and destroy the body’s healthy cells, tissues, or organs. The immune system attacks the body because it cannot differentiate between viruses, bacteria, germs, and healthy cells. In simple terms, the body is destroying itself in a misguided attempt to protect itself from disease.
There are four types of lupus:
- Systemic lupus – (Approximately 70 percent of all cases of lupus) Affects a major organ or tissue in the body, such as the heart, lungs, kidneys, or brain in roughly half of these cases
- Cutaneous lupus – (Approximately 10 percent of all cases of lupus) Affects only the skin
- Drug-induced lupus – (Approximately 10 percent of all lupus cases) Caused by high doses of certain medications. The symptoms of drug-induced lupus are like systemic lupus; however, symptoms usually subside when the patient stops using the medications
- Neonatal lupus – A rare condition in which the mother’s antibodies affect the fetus. At birth, the baby may have a skin rash, liver problems, or low blood cell counts, but these symptoms typically disappear completely after six months with no lasting effects
Some of the signs and common symptoms of lupus
Common symptoms of lupus include joint pain, extreme fatigue, hair loss, a “butterfly” skin rash, chest pain, dry eyes, trouble breathing, headaches, confusion, memory loss, oral ulcers and high sensitivity to sunlight. These symptoms, often referred to as “flare-ups,” can pop up and go away for days, months, and even years.

Common symptoms of lupus include joint pain, extreme fatigue, hair loss, a “butterfly” skin rash, chest pain, dry eyes, trouble breathing, headaches, confusion, memory loss, oral ulcers and high sensitivity to sunlight
They vary from person to person, with no two people having the same symptoms. A person’s symptoms can even change over time. The symptoms of lupus are so varied that 333 people in a room may have lupus, with no one having the same presentation.
Patients with lupus must be vigilant and pay attention to what they consume as it could affect their health. They can’t just take any herb or vitamin as there is a possibility it could conflict with their treatment.
In addition, patients must monitor every symptom that occurs, as any slight fluctuation could signal a flare-up. For example, patients with lupus may experience painless mouth sores, which many people may be tempted to overlook. This, however, could be an early sign of a flare-up.
Another common symptom of lupus is constant fatigue. No matter how much sleep the patient gets, it never seems enough.
As of today, there is no single test that can diagnose lupus. The autoimmune antibody test (ANA), a blood test used by doctors to measure the activity of your immune system against specific foreign invaders, can give out false positives. Meaning people with other diseases or even no disease at all may test positive.
Some people can have lupus and test negative with the ANA test. Because of this, there is a combination of symptoms, tests, and physical exams necessary for a patient to be diagnosed with lupus.
Due to the complexity of the disease, patients with lupus cannot leave the management of their disease solely to the care of health professionals. They must take a very active role.
What does the lupus rash look like on dark skin?
One very common symptom of lupus is a rash. It’s thought that rashes occur in patients with lupus when they have been exposed to sunlight. The UV radiation damages the cells in the skin and exposes antigens that the immune system recognizes. This leads to an immune response in the skin. Generally, on black or brown skin, a widespread rash can look like a viral rash. It can resemble flat or raised dots that are brown, purple, or black.
There are different lupus rashes:
Malar (or butterfly): An acute cutaneous lupus rash happens when systemic lupus is active. It appears around the cheekbones and has the shape of a butterfly as it goes across the bridge of the nose.
This rash can also occur on the arms, legs, and body. Like most lupus rashes, this rash is generally inflamed and raised. In brown and black skin, it can appear as red, brown, or darker than the original skin color.
Circular Rash (discoid lupus): A type of chronic cutaneous lupus with the round shape of sores or lesions. The patches are thick, raised, and scaly. On people with dark skin, instead of appearing pink, the patches look darker.
These rashes can appear on the face, ears, scalp, neck, and hands. They are not usually itchy or painful but can cause pigment changes such as white or discolored patches or possibly scarring after the rash has cleared.
Subacute cutaneous lupus lesions: Papulosquamous and annular lesions fall into this category of lupus rashes/lesions. They are very photosensitive but not itchy or painful, nor do they leave scars.
Papulosquamous lesions are usually red scaly areas and appear on the shoulders, back, and chest. Annular lesions resemble fungal infections. That is, they are circular and have ring-type patterns.
Challenges women of color face with lupus
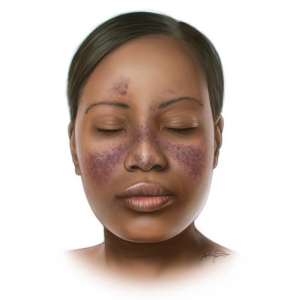
Malar, or butterfly, is an acute cutaneous lupus rash that happens when systemic lupus is active. It appears around the cheekbones and has the shape of a butterfly as it goes across the bridge of the nose.
According to the Centers for Disease Control and Prevention, nearly 1.5 million Americans have lupus, with nine out of 10 being women between the age of 15 to 44 (childbearing age). Black women make up most of the people living with lupus, as the disease affects them two to three times more than white women.
A study by the University of Michigan researchers found that 1 in 537 Black women were diagnosed with lupus compared to one in 1,153 white women.
With so many suffering from this disease, it is shocking that it takes nearly six years from when people with lupus first notice symptoms until they get a correct diagnosis, as studies have shown. The Lupus Foundation of America conducted a study of over 3,000 adults with lupus and found that nearly 40 percent of them waited more than one year from the onset of symptoms to receive an accurate diagnosis.
Of the people surveyed, 46.5 percent reported being misdiagnosed with something other than lupus at the start of their journey with this disease, while 54.1 percent were told that nothing was wrong with them or that their symptoms were psychological.
Another challenge Black women face regarding living with lupus is the need for child or elder care. While family support proves to be a significant source of advocacy regarding pushing for proper medical care, it also proved to be a considerable hindrance to adherence to the medical regimen and medical appointments. Black women gave challenges with finding elder and child care as the primary reason for missing medical appointments.
Challenges Black men face with lupus
While only one in 10 lupus patients are men, research shows that certain symptoms are more pronounced in men than in women. For example, men who have kidney complications with lupus tend to have more severe challenges.
Another unfortunate difficulty men must contend with is the false assumption that the disease only affects women. Because of this, men experience even longer delays in getting a proper diagnosis, even when they show symptoms. This is probably why they tend to be older than women when they finally get diagnosed, as some research indicates.

While only one in 10 lupus patients are men, research shows that certain symptoms are more pronounced in men than in women.
The cost of delayed care and misdiagnosis
According to a 2015 paper published in the “Annals of the Rheumatic Diseases,” on average, lupus patients delayed seeking medical attention for over two years from when they first started noticing symptoms. When they sought medical attention, the lack of knowledge about the disease caused them to be misdiagnosed, told nothing was wrong with them, that their symptoms were psychological, or outrightly accused of seeking drugs. This inadvertently leads to misdiagnosis and delays in proper diagnosis and treatment, causing permanent organ damage.
A study titled “Delayed diagnosis adversely affects outcome in systemic lupus erythematosus: Cross sectional analysis of the LuLa cohort” supports the findings of the 2015 paper, showing that the longer the length of time between when a patient first starts experiencing symptoms to when they are actually correctly diagnosed, the higher the disease activity, disease-related damage and fatigue, and the lower the health-related quality of life.
Early diagnosis not only dramatically improves the outcome of patients with lupus, but it also reduces the risk of patients developing life-threatening problems, such as a heart attack or stroke.
Treatment options for lupus
Currently, there is no cure for lupus, but there are promising treatment options for patients. One such option is Stem Cell Transplant Therapy.
Everyone has stem cells in their body. As we age, so do these cells, and the number and effectiveness of our stem cells decrease as time passes. In this treatment, a lupus patient is administered with genetically intact stem cells usually obtained from a fetus.
Stem cells can also be obtained from the patient if the cells have not been affected by the disease. Because stem cells can turn into the cells of damaged organs when they touch said organs, they are effective in treating lupus. In fact, stem cells similarly treat damaged nerves and muscles, causing a reduction in the progression of the disease.
For more than 10 years, doctors have been treating lupus patients with stem cells. It has shown to be highly effective in stopping the autoimmune disease process, leading to sustained remission. This treatment has been especially effective for people who don’t respond to other lupus treatments.
Depending on the patient’s condition, this treatment can be performed in three sessions, 45 days apart, or in three consecutive days. If the disease has significantly advanced, the treatment may need to be repeated on the patient more than once.
Knowledge is the key to better healthcare
Since the Black community is understandably distrustful of healthcare and medicine in the United States, they must equip themselves with the necessary knowledge to safeguard their health and advocate for their care. Lupus sheds a glaring light on this lapse, as the statistics above reveal. The only way to fight against lupus is to be equipped with knowledge of the disease, its various symptoms, and possible treatments.
Increased knowledge about this autoimmune disease would drastically reduce these challenges. Patients would recognize their symptoms and seek medical attention faster. The rate of misdiagnosis or dismissing patients’ complaints would decrease, and proper tests to diagnose the disease would occur more swiftly because doctors have a better understanding of the different ways the disease presents itself.
With more information and education about lupus, the Black community would be better able to support people living with the disease as they navigate their care while balancing familial responsibilities. For the Black community, the key to navigating lupus is better knowledge of the disease, increased outreach and awareness in the healthcare system, and stronger advocacy for more inclusive medical research and treatment.
Yolanda Goodloe Cowart is an author, small business champion, victims advocate, civil rights activist, and human rights defender in St. Petersburg-Clearwater.