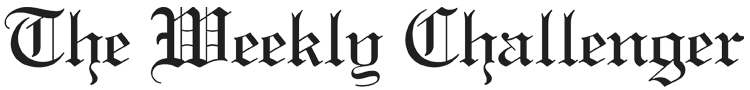Jessica Estévez, co-founder of Estrategia Group, and Galo Cruz, a medical case manager at EPIC, sat down with The Weekly Challenger to discuss HIV awareness and prevention in the Pinellas Latinx community.
J.A. JONES, Staff Writer
ST. PETERSBURG – Most recent Pinellas County health data shows that Latinx (Hispanic) communities in Pinellas County consistently had higher rates of new HIV cases compared to non-Hispanics. Additionally, Latinx people have had a five percent increase in the rate of new HIV cases since 2015.
The CDC stated that if the rates of HIV diagnosis among the Latinx population in the U.S. continues to rise and if current rates persist, one in five Latinx gay and bisexual men, one in 48 hetero men, and one in 227 Latinx females may be diagnosed with HIV in their lifetime.
Many of the same health disparities and equity issues that plague Black communities are found in Latinx (Brown) communities, including poverty, inadequate education, poor distribution of medical resources, and medical mistrust.
Additionally, a language barrier exists – while the “cultural value” of machismo inhibits open conversation around down-low behavior, as does religious mores. Both of these have negatively impacted testing among Latinx people as well.
While the term “Latinx” groups people whose roots lie in various Spanish-speaking countries under one title, health data indicates that behavioral risk factors for HIV actually vary from one country to the next.
For instance, Latinx people born in Puerto Rico are most likely to contract HIV from intravenous drug use (IDU). At the same time, research shows the primary cause of HIV in Latinx men born in Mexico or the U.S. is sexual contact with other men.
Recently, Jessica Estévez, co-founder of Estrategia Group, and Galo Cruz, a medical case manager at EPIC, sat down to discuss HIV awareness and prevention in the Pinellas Latinx community.
Cruz was born and raised in Puerto Rico before relocating to Philadelphia, and finally, St. Pete. He works closely with Spanish language clients who may have language barrier issues, helping them complete their paperwork to determine eligibility for services and set up medical appointments and medication.
He also educates clients and community members on the role of CD4 cells in our immune system. CD4 cells, also called T-cells, are white blood cells that destroy bacteria, viruses and invading germs in our body.
Cruz shared how HIV attacks the immune system by attacking the CD4 cells, enabling the HIV viral load in the body. He noted that the role of HIV medication is to suppress the viral load in one’s body. “At the beginning, the viral load is high, CD4 is really low — but when you start taking the medication, CD4 goes up.”
Estévez acknowledged possible confusion surrounding HIV and AIDS terminology; while HIV, human immunodeficiency virus, can become AIDS, acquired immunodeficiency syndrome, if untreated, many are unaware of the difference.
Noting that it’s easy to get “lost” in terminology, she asked Cruz to share insight into how HIV education was being communicated in the Latinx community.
“It’s sad to say, but I consider the Latino community like a sleeping giant, in the case of HIV AIDS,” Cruz admitted, noting that the statistics were “painful” – including the fact that among older Latinx people, AIDS had become the fourth leading cause of death, and the sixth leading cause among younger Latinx people.
He cited obvious factors, including lack of education: “For instance, patients go to a doctor, and don’t see many bilingual staff. When [English- speaking staff] start talking in clinical terms, Spanish speakers get lost.”
Cruz also noted that often people are afraid to seek help because of their immigration status. “Some people are afraid that, ‘if I go to the hospital, I might be deported to my country’ — and they refuse to go or seek medical attention until late; when they find out, they are diagnosed with AIDS.”
People can have HIV for five to ten years before it actually becomes full-blown AIDS, and Cruz explained that an AIDS diagnosis comes down to numbers. “If your CD4 count falls below 200, even one time, it’s considered AIDS because your immune system is weak. And because your immune system is weak, and you can have different diseases than normal people can.”
But he added, “If you are HIV positive, but your CD4 count is over 300, it’s not considered AIDS. That’s why I try to educate my community — don’t be scared about the number — because in many cases, people with their CD4 count below 200 starts taking the medication, and raise their CD4 count to over 800 or 1000, and they can live healthy, better lives.”
Estévez focused on possible areas where those seeking support regarding HIV status can go in the Latinx community. Cruz noted that while prevention programs such as EPIC connect individuals with numerous services, a church can also be a place of support that can promote healthy lifestyles.
He also shared the strength and importance of familial support, specifically sharing the idea that “Something similar in Latino and African-American communities is [trust in] Grandma — whatever Grandma says,” is vital in creating a supportive environment for those in crisis.
Noting that “many of the HIV cases patients feel alone — like they don’t have support,” Cruz shared that faith-based organizations should make a greater effort to “let them (HIV patients) know we don’t exclude people, we include people – that you’re part of the community, and you’re important.”
Growing up as a Latinx youth, he realized there was a taboo about sex. “I never remember my mom talking about sex. And in church, people are afraid to talk about sex.” Also complicating the issue, said Cruz, is that the “machismo” ethic in Latinx cultures adds to a silence that is similar to the Black community’s “down-low” (hidden bi-sexual behavior) activity.
Cruz noted that there is a tendency to talk about apocalyptic, end-time events among some religious circles in Latinx churches. “Many just see HIV/AIDS as a punishment from God, or a symbol of the end of the world. As Latinx people, we have to communicate that God loves everyone, and God does not exclude — he wants us to work together.”
To learn more about HIV support services available at EPIC, visit myepic.org. You can also view the entire conversation between Cruz and Estévez on The Weekly Challenger’s YouTube channel.